We often tend to associate some eating behavior with a state of mind. Are we sad? We tend not to eat. Are we happy? We eat a lot. How our moods can influence our relationship with food is an extraordinarily complex topic. Because of its complexity, it would require a separate chapter in this overview.
But if our moods influence our behaviors and our “food cravings,” is the reverse also true? Can what we eat influence our behaviors?
Fiber and health
Nowadays, given their success, everyone is aware of the extraordinary properties of fiber and the benefits associated with its consumption.
But what is fiber? It is polysaccharides not directly usable by the human body but used by intestinal bacteria as a source of sustenance and nutrition. Depending on the ability to retain water, fiber can be classified into:
- soluble fiber (gums, mucilage, pectin, beta-glucans, fructooligosaccharides, galactooligosaccharides, and inulin);
- insoluble fiber (cellulose, hemicellulose, and lignin).
Soluble and insoluble fibers act slightly differently. However, both bring various benefits to the body since, in most fruits, vegetables, cereals, and legumes, we find a mix between the two categories (Fig. 1).

What are the benefits of fiber?
- It improves intestinal transit;
- Fiber favors evacuation by contrasting constipation;
- Fiber increases the sense of fullness, contributing to weight loss;
- It reduces the absorption of lipids and carbohydrates. In this way postprandial glycemic peaks are avoided, and there is a lowering of LDL cholesterol and glucose levels in the blood. The consumption of fiber is, therefore, useful to counteract the development of type 2 diabetes mellitus
Last but not least, from the fermentation of fiber by intestinal bacteria are produced short-chain fatty acids (SCFA). These fatty acids have immunomodulatory and immunostimulant activity, act as nutrition for colonocytes and are also essential for the well-being of the brain.
Fiber is a key component of a healthy diet. Daily consumption of 25/30 g of fiber seems to be the panacea for many ills. It helps to counteract the onset of cardiovascular diseases, diabetes and metabolic syndrome, digestive diseases (diverticulosis) and helps to reduce inflammatory processes associated with many diseases.
The Fiber-Depression nexus
A healthy microbiota and a rich and varied diet are two factors that play a key role in brain development and function. The World Health Organization has predicted that starting in 2020, depression will be one of the largest and most influential causes of weight gain or loss for society.
Coupled with this, the increased consumption of refined foods and the increasingly strict adherence to a Westernized diet is contributing to the spread of obesity and the onset of all the problems that come with it.
Is it possible that these two trends intersect?
In recent years, several researchers have ventured into understanding how diet affects our emotions. The focus of these studies is precisely fiber.
In particular, a diet rich in fruits and vegetables is associated with greater psychological well-being and a reduced risk of depression. This result was associated not only with the consumption of fruits and vegetables but also with the use of whole grains that are, as we know, rich in fiber.
Longitudinal studies have shown that the consumption of refined foods and high amounts of sugary foods seems to be associated with an increased risk of depression. This effect, however, could be associated with the overall diet and lifestyle of the study participants but… can fiber be the key?
The glycemic index also plays a role.
A fundamental contribution to this hypothesis is provided by an observational and longitudinal study carried out on 93,676 postmenopausal women, monitored for 4 years.
The starting point of this study was the hypothesis that a high glycemic index (typical of many refined and low-fiber foods, Fig. 2) could be associated with a higher prevalence of depressive disorders. Researchers also examined the association between fiber consumption and specific foods (whole and nonwhole grains, fruits, vegetables, nuts, seeds, and legumes) and the incidence of depression.
The final analysis showed that consumption of foods with a high glycemic index was associated with higher body mass index, lower physical activity, and lower consumption of fiber, fruits and vegetables, legumes, and nuts. Depression would also appear to be associated with all of these factors, including lower fiber intake.

Could the two be related?
Since a diet high in fiber slows down carbohydrate metabolism and lowers the glycemic index of certain foods, the association between a lower incidence of depressive disorders and increased fiber consumption could be due to the ability of fiber to influence the glycemic index of foods.
It works, but only in the short term (and at what cost?).
Going back to the initial point, individuals suffering from depression tend to consume a high amount of sugar as a palliative for the depressive state. We know that this mechanism, in the short term, works. The consumption of carbohydrates would seem to favor the synthesis of serotonin in the brain, while insulin released following the meal would favor the increase of tryptophan in the plasma and, consequently, would contribute to the increase of serotonin synthesis.
This effect is mainly obtained after a meal consisting almost and exclusively of carbohydrates… but how happy are we when we eat a nice gummy candy?
The pleasure of eating sweet foods could give temporary relief, but be careful not to abuse it!
What are the mechanisms at the base of the relationship depression – fiber – glycemic index? The plausible mechanisms behind these relationships could be multiple. First of all, the high consumption of highly refined foods and simple sugars is an important risk factor for cardiovascular disease. This also underlies many inflammatory processes, factors associated with the pathogenesis of depression.
The role of inflammation
Another fundamental aspect of the fiber-depression nexus concerns inflammation. Already in 1990 a possible link between inflammation, especially chronic low-grade inflammation, and depression was proposed…. but let’s start with fiber.
Some studies have observed that higher fiber consumption is associated with a reduction in chronic inflammation characteristic of some cardiovascular diseases, type 2 diabetes, and metabolic syndrome. Specifically, in subjects on a low-fiber diet, there was an increase in some markers of inflammation including C-reactive protein, interleukin-6, and leptin.
In contrast, increased fiber consumption was associated with a lower concentration of leptin, lowered serum levels of C-reactive protein, and increased adiponectin, an adipokine produced in adipose tissue that is generally considered anti-inflammatory.
Inflammation as mediator
As mentioned above, depression, also because of a particular relationship that is established with food, is associated with increased cardiovascular risk, metabolic syndrome, and, indirectly, increased chronic inflammation resulting from it.
In fact, in subjects suffering from depression, it has been observed an increase in the levels of C-reactive protein (CRP), interleukin 1 (IL-1), interleukin 6 (IL-6), and tumor necrosis factor-alpha (TNF-alpha), as well as a lowering of adiponectin levels. Chronic inflammation would thus appear to be implicated, in part, in the pathogenesis of depression.
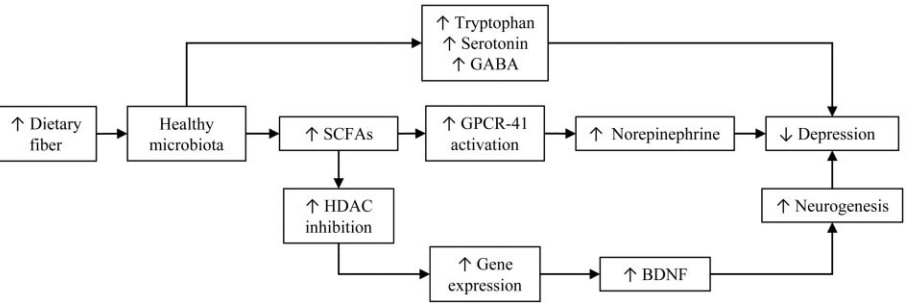
Since fiber would appear to influence the levels of various markers of inflammation, and inflammation could contribute to the pathogenesis of depression, the link between fiber consumption and depression could be in part mediated by inflammation itself (Fig. 3).
Conclusions
However, we must consider that the relationship between depression and consumption of highly refined and sugar-filled foods is bidirectional. Depressive behaviors lead subjects to binge on foods that, at that moment, cause a certain comfort … and what better than large quantities of pizza, juices, chips, and so on?
There is still a long way to go, as many mechanisms underlying inflammation and depression itself are not yet fully understood. Moreover, these effects could also be linked to the presence of compounds such as polyphenols, vitamins, and minerals. In addition, other factors such as gender, age, level of physical activity, and individual lifestyle could also contribute to the pathogenesis of inflammation and depression.
Higher fiber consumption could therefore influence chronic inflammation states and, indirectly, depressive behaviors. But further studies are certainly needed. What is known for sure is that consuming 30g per day of fiber is beneficial to the body.
Original article: Alimentazione e depressione: il ruolo delle fibre – Microbiologia Italia by Ilaria Salvatori
Bibliography
- Dietary fiber and its associations with depression and inflammation – PubMed (nih.gov)
- Exploration of the association between dietary fiber intake and depressive symptoms in adults – PubMed (nih.gov)
- Association of dietary fiber and depression symptom: A systematic review and meta-analysis of observational studies – PubMed (nih.gov)
- Linee guida per una sana alimentazione (2018) – CREA